Advertisement
As U. S. Hospitals Prepare Ebola Response, Nurses Must Have A Seat At The Table
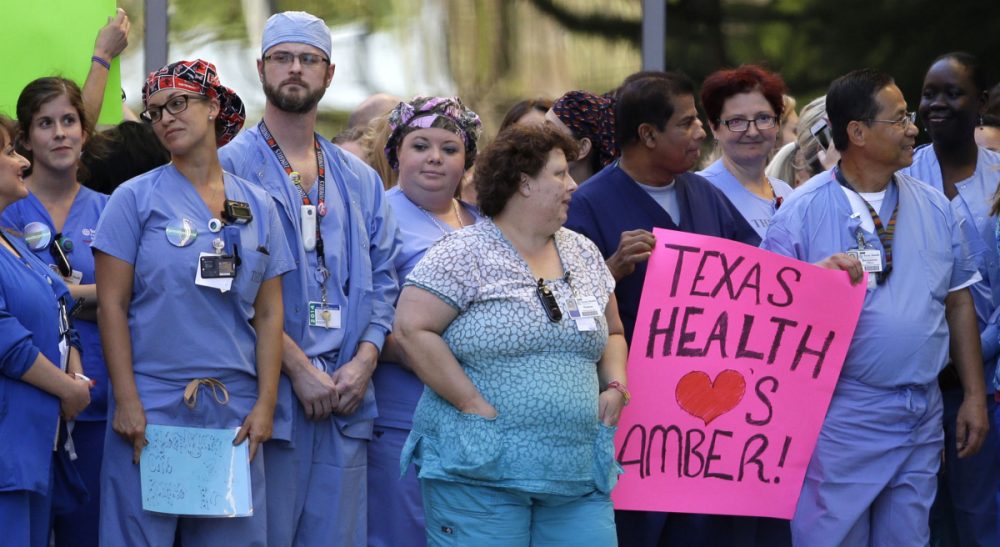
If there is a silver lining in the current Ebola crisis, it's that workplace safety for health care workers is finally getting public attention . For a brief time last week, the world was focused on nurses, seeing both the necessity of their role and the hazards of their work.
Amid the widespread and understandable public concern about possible contagion, one critical fact keeps being shunted aside: The only two Ebola transmissions inside the U.S. have been nurses who were infected at work, performing their regular duties.
Nurses are the front line of care. They are directly affected by infectious disease risks. They have firsthand knowledge of the day-to-day details of caring for an ill patient, a process that affects the health of both patients and nurses.
There has been a lot of blame directed at the hospital staff that initially sent Thomas Eric Duncan, the first person to die of Ebola in this country, home from a hospital in Dallas, Texas. There has been no shortage of coverage of the two nurses, Amber Joy Vinson and Nina Pham, who contracted Ebola from him. The media has, however, largely ignored the organizational context in which Vinson and Pham and other nurses like them were working.
Nurses are the front line of care. They are directly affected by infectious disease risks. They have firsthand knowledge of the day-to-day details of caring for an ill patient, a process that affects the health of both patients and nurses. However, in times of crisis, nurses are often excluded from decision-making conversations at every level of health care organizations, from patient care decisions to hospital policy and protocols.
Nonfatal workplace injury and illness rates among nursing staff are 7.6 per year for every 100 workers. This rate is twice as high as that for construction workers, with 3.7 injuries per 100 workers. The wide range of risks faced by nurses and nursing assistants includes infection by blood- and airborne pathogens, musculoskeletal injuries from lifting patients and other tasks and verbal and physical assault. The potentially lethal risk presented by caring for an Ebola patient is but one example of the risks faced by these workers every day.
Yet media and governmental inclusion of nurses’ voices has been practically nonexistent. Only recently have Dallas nurses begun to speak out about care at their hospital. In Massachusetts, an Oct. 16 legislative hearing on Ebola initially excluded nurses from testifying, although this pronouncement was retracted shortly before the session.
The exclusion of people who best understand the risks seems to be a recurring problem in the Ebola conversation. Occupational safety and health specialists are being ignored, as well. These professionals have detailed knowledge about how aerosols are created and spread in indoor spaces; how to put on and take off protective clothing correctly; and how the general workplace climate affects people’s behaviors. Occupational health researchers studying health care institutions have repeatedly called attention to the systemic nature of many safety problems and the importance of engaging workers fully in developing preventive programs to optimize their effectiveness.
Advertisement
Although many hospitals and states are gearing up for a response to Ebola, there is still little evidence that direct care nurses and other clinical staff members have a seat at the table when it comes to developing specific practices and policies. This omission did not begin with Ebola, and it will not end when the current crisis is over. Some of this is the consequence of the nursing profession’s gendered history.
For most of the 20th century, the female-dominated profession of nursing was subservient to the male-dominated occupation of doctoring. Women are becoming physicians in increasing numbers, but nursing work remains more than 90 percent female and the power hierarchy of health care remains unchanged. In fact, the stratification of the health care workforce has been exacerbated in recent decades by the dramatic expansion of a low-wage army of nursing aides and assistants who have even less voice in their workplaces than nurses do.
Although many hospitals and states are gearing up for a response to Ebola, there is still little evidence that direct care nurses and other clinical staff members have a seat at the table when it comes to developing specific practices and policies.
The “caring” element of nursing work inherently demands that these workers put their patients’ needs ahead of their own. In male-dominated occupations, such as firefighting and law enforcement, where this is the norm, these people are hailed as heroes. When a firefighter is injured or dies in the line of duty, it is appropriately seen as a tragedy. Mistakes are analyzed to understand what could have been done better and what changes could protect safety in the future. It is rare, however, that blame is cast upon injured workers, especially publicly. But Amber Joy Vinson and Nina Pham, who set aside fear for their own safety to care for Thomas Eric Duncan, their patient, were publicly charged with carelessness. One wonders if the gendered nature of nursing work results in such different treatment.
Instead of blaming nurses, let’s use the spotlight of the Ebola crisis to highlight the workplace safety issues that they face every day. Let’s change the governance structure of hospitals and other health care organizations to support the full participation of nursing and other direct care workers in the problem-solving process, so that the implemented approaches provide the best chance of safety for both workers and patients.
This article was co-authored by the University of Massachusetts, Lowell's Laura Punnett, professor of Work Environment; Mignon Duffy, associate professor of Sociology; and Alicia Kurowski, post-doctoral fellow at the Center for the Promotion of Health in the New England Workplace.
Related:
